Why your retina can reveal cardiovascular risk long before you feel unwell.
High blood pressure is one of the most common — and most dangerous — health conditions in South Africa and worldwide. Yet millions of people don’t know they have it. Symptoms often appear only once severe damage has already occurred.
But there is one place in the body where early damage becomes visible long before patients feel anything: the retina.
Because the retina contains tiny blood vessels that respond directly to changes in blood pressure, your eyes can reveal early warning signs of hypertension that your heart, brain or kidneys may not show yet. For GPs and optometrists, these retinal changes are often the first clue that a patient’s cardiovascular system is under strain.
This article explains how hypertensive retinopathy develops, why retinal exams are essential for early detection, and how closer collaboration between GPs and ophthalmologists leads to better outcomes for patients aged 40 and above.
View VideoWhy the Retina Gives Clues You Can’t Get Anywhere Else
The retina is the only place in the body where clinicians can directly observe blood vessels without surgery. When blood pressure is elevated over time, those vessels begin to change in predictable ways.
These changes offer three crucial insights:
They reveal long-term blood pressure trends
Even if a patient’s blood pressure is normal during a single reading, retinal changes can show whether hypertension has been present for months or years.
They reflect systemic vascular health
Damage seen in the retina often mirrors what’s happening in the heart, kidneys, and brain.
They provide early warning signs
Patients may feel fine, yet retinal damage is already underway — making eye exams one of the most valuable early detection tools.
For patients over 40, where hypertension risk rises significantly, regular retinal exams are not merely about eye health but overall health.
Understanding Hypertensive Retinopathy Symptoms (Stages & Meaning)
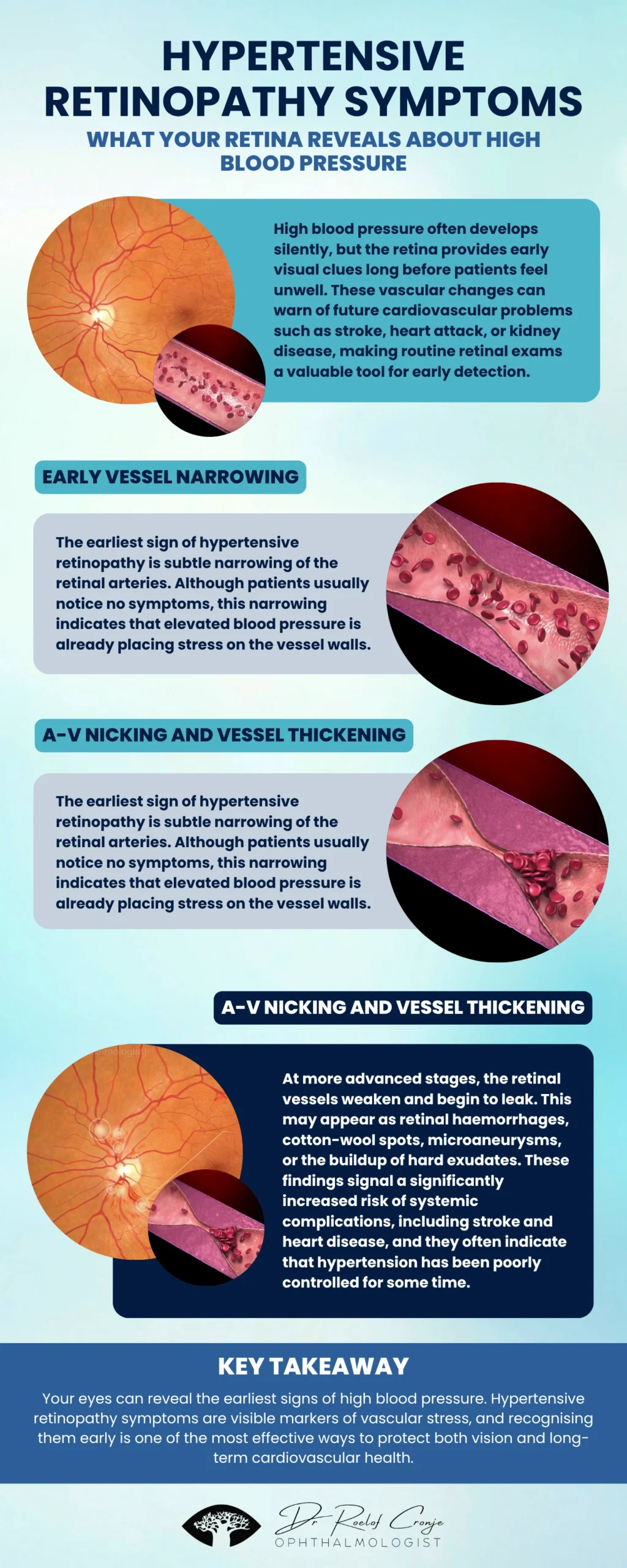
Hypertensive retinopathy occurs when high blood pressure damages the tiny blood vessels in the retina. These changes progress through distinct stages that help clinicians identify the severity of systemic hypertension.
Below is an easy-to-understand breakdown suitable for both clinicians and patients.
View VideoStage 1 — Mild: Subtle Vessel Narrowing
The earliest hypertensive retinopathy symptoms include:
- Generalised narrowing of retinal arteries
- Slight reduction in vessel flexibility
Patients experience no symptoms, and this stage is usually detected only during routine eye exams. It signals early or persistent elevated blood pressure.
Stage 2 — Moderate: A-V Nicking and Vessel Wall Thickening
With ongoing hypertension, arteries thicken and begin to compress crossing veins — known as arteriovenous (A-V) nicking. This is one of the most common findings during optometric or ophthalmology exams.
It indicates moderate, long-standing hypertension that is beginning to cause structural vessel changes.
Stage 3 — Severe: Leakage, Haemorrhages & Cotton-Wool Spots
At this stage, high blood pressure has weakened vessel walls, leading to:
- Retinal haemorrhages (“bleeding” spots)
- Microaneurysms
- Cotton-wool spots (areas of reduced blood flow)
- Hard exudates (fatty deposits from leaking vessels)
These findings are strongly associated with increased risk of stroke, heart attack, and kidney disease.
Patients may begin to notice blurred or fluctuating vision, but many still feel no systemic symptoms.
Stage 4 — Malignant Hypertension: Optic Nerve Swelling
This is a medical emergency.
Dangerously high blood pressure causes swelling of the optic nerve (papilloedema), which can rapidly damage vision and is often accompanied by:
- Severe headaches
- Nausea
- Visual disturbances
Immediate hospital care is essential — this stage is life-threatening.
Why Retinal Exams Should Be Part of Every Hypertension Check (Especially 40+)
A retinal exam is far more than an eye test — it is a vascular health assessment.
View VideoFor Patients Over 40
Retinal imaging can:
- Detect early hypertensive retinopathy symptoms before you feel ill
- Prevent sudden or permanent vision loss
- Provide clear evidence of how well your treatment is working
- Reveal cardiovascular risks you may not know you have
- Motivate lifestyle and medication adherence
Patients often say, “Seeing my eye vessels made the problem real for me.”
For GPs and Optometrists
Retinal findings provide:
- Objective evidence of vascular damage
- A powerful tool for hypertension risk stratification
- Guidance on treatment urgency
- A visual way to educate and motivate patients
- A trigger for referral to an ophthalmologist when needed
A simple image can change a patient’s outlook entirely.
When Should a GP or Optometrist Refer a Patient?
Referral to an ophthalmologist is recommended when:
- Any retinal haemorrhages, exudates, or cotton-wool spots are present
- Vision is affected or fluctuating
- Hypertension is newly diagnosed or poorly controlled
- Malignant hypertension is suspected
- The patient has comorbidities like diabetes or kidney disease
- Fundus imaging shows progression between visits
Early referral can prevent vision loss and reveal broader systemic risks.
The Power of Collaboration: GPs, Optometrists, and Ophthalmologists Working Together
Hypertension is a lifelong condition affecting every organ system. The retina often shows the earliest signs of damage, making eye care an essential part of hypertension management.
When GPs, optometrists, and ophthalmologists collaborate, patients benefit from:
- Earlier detection of high blood pressure
- Better monitoring of treatment success
- Prevention of severe complications
- Reduced risk of stroke and heart attack
- Early intervention for vision-threatening changes
Retinal imaging is not optional — it’s a crucial component of holistic cardiovascular care.
Conclusion
Your eyes provide a window into your blood vessels — and into your overall cardiovascular health. Hypertensive retinopathy symptoms often appear long before patients feel unwell, making regular retinal exams one of the most powerful early-detection tools available.
For clinicians, these retinal changes provide vital information that can shape treatment decisions. For patients over 40, they offer an early warning and an opportunity to protect both vision and long-term health.