A Clinician’s Quick-Reference Guide for Primary Care and Emergency Settings
In general practice and emergency medicine, eye complaints account for up to 3% of all consultations — yet a small percentage of these represent sight- or even life-threatening emergencies. The difference between recovery and irreversible blindness often lies in a few key decisions made at first contact.
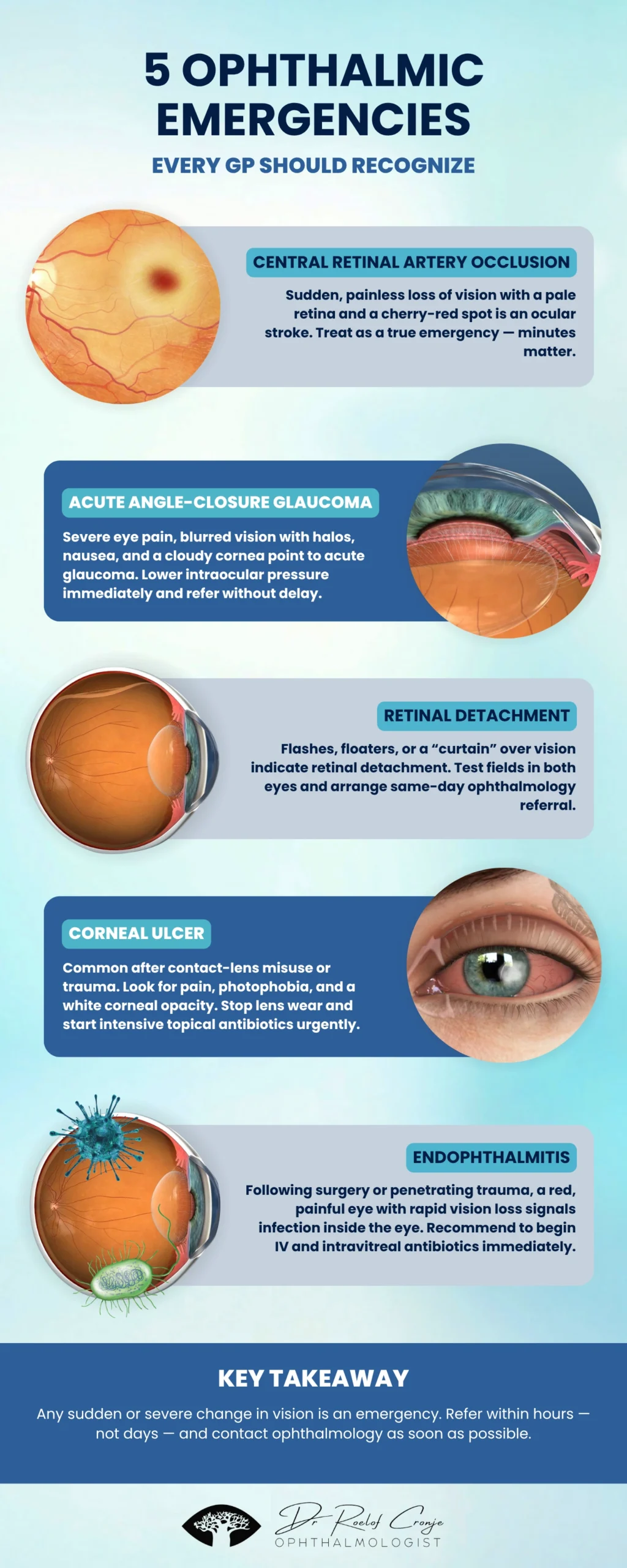
This practical guide outlines the five most critical ophthalmic emergencies every GP should recognize, what to look for, and what immediate steps to take before referral.
1. Central Retinal Artery Occlusion (CRAO)
Presentation:
- Sudden, painless, profound loss of vision in one eye
- Onset often upon waking or during exertion
- Relative afferent pupillary defect (RAPD) present
- Fundoscopy: pale retina, cherry-red fovea, narrowed arterioles
- May have history of hypertension, diabetes, or carotid disease
Pathophysiology:
Blockage of the central retinal artery (usually embolic) leads to retinal ischemia and cell death within 90–120 minutes.
Immediate GP Management:
- Record visual acuity and pupils (both eyes).
- Call ophthalmology and neurology immediately — treat as a stroke equivalent.
- Check blood pressure, glucose, and cardiac rhythm.
- Initiate stroke protocol: consider urgent carotid imaging and ECG.
- If ophthalmology not immediately available, brief measures such as ocular massage or acetazolamide (500 mg PO/IV) may be attempted — but must not delay referral.
Key Point:
View VideoCRAO = ocular stroke. Urgent multidisciplinary management is essential for vision and systemic outcomes.
2. Acute Angle-Closure Glaucoma (AACG)
Presentation:
- Sudden, severe eye pain often radiating to the head or jaw
- Blurred vision, halos around lights
- Nausea, vomiting, and malaise (often misdiagnosed as migraine or gastroenteritis)
- Eye is red, cornea steamy, pupil mid-dilated and fixed
- Globe feels rock hard on gentle palpation
Pathophysiology:
Blockage of aqueous outflow through the trabecular meshwork causes rapid intraocular pressure (IOP) rise and ischemic damage to the optic nerve.
Immediate GP Management:
- Do not delay referral — this is a true emergency.
- Avoid mydriatic drops or patching the eye.
- If specialist access is delayed:
- Acetazolamide 500 mg PO or IV (if not contraindicated)
- Topical timolol 0.5% and apraclonidine 0.5%, if available
- Control pain and nausea
- Arrange same-hour ophthalmology review for laser iridotomy or medical decompression.
Key Point:
View VideoA red, painful eye with blurred vision and systemic symptoms = acute glaucoma until proven otherwise.
3. Retinal Detachment
Presentation:
- Sudden onset of flashes (photopsia), floaters, or “a shadow” in the peripheral vision
- May progress to a dark curtain or veil
- Vision typically painless but progressively lost
- Fundoscopy: detached retina appears grey, mobile, and undulating
Pathophysiology:
Retinal separation from the retinal pigment epithelium — usually from a retinal tear allowing vitreous fluid to accumulate underneath.
Immediate GP Management:
- Do not apply pressure to the globe.
- Check visual acuity and confrontational fields.
- Keep the patient upright and still (reduces retinal spread).
- Urgent same-day referral to ophthalmology.
- If macula still attached (“macula-on detachment”), surgical repair within 24 hours gives best outcomes.
Red Flags:
- Sudden showers of floaters
- Photopsia in low light
- Monocular field loss
Key Point:
View VideoAny “flashes and floaters” in a high-risk patient (myopia, trauma, diabetic retinopathy) = same-day referral.
4. Corneal Ulcer (Microbial Keratitis)
Presentation:
- Painful red eye, photophobia, tearing, foreign-body sensation
- Blurred vision or white spot on the cornea
- Often contact-lens related, especially overnight wearers
- Fluorescein staining: focal corneal infiltrate/ulcer, epithelial defect, surrounding edema
Pathophysiology:
Microbial invasion (commonly Pseudomonas in lens wearers, Staph aureus or fungi post-trauma) leads to stromal necrosis and potential perforation.
Immediate GP Management:
- Urgent ophthalmology referral — same day.
- Never patch the eye or use topical steroids.
- Stop contact lens use immediately.
- If referral delayed:
- Start topical fluoroquinolone (ciprofloxacin 0.3% or ofloxacin 0.3%) hourly.
- Educate patient on hygiene, risk of perforation, and need for cultures.
Key Point:
View VideoPain + corneal opacity = never just “pink eye.” Always treat as an emergency.
5. Endophthalmitis
Presentation:
- Severe ocular pain, rapid vision loss, redness, photophobia
- Often occurs days after intraocular surgery, intravitreal injection, or penetrating trauma
- Slit-lamp/ophthalmic exam: hypopyon, vitritis, reduced red reflex
Pathophysiology:
Bacterial or fungal infection within the vitreous cavity causes widespread inflammation and irreversible tissue destruction.
Immediate GP Management:
- Emergency ophthalmology contact — this is a true sight-threatening emergency.
- Do not delay for imaging or systemic antibiotics (intravitreal therapy needed).
- Record vision and note timing of recent ocular procedures.
- If discharge or culture collection possible before transfer, do so.
Key Point:
Any post-surgical patient with pain, redness, or cloudy vision = endophthalmitis until proven otherwise.
Summary: GP Quick-Action Table
| Condition | Key Signs | Immediate Action | Why It Matters |
|---|---|---|---|
| CRAO | Sudden painless vision loss, cherry-red spot | Urgent ophthal/neuro referral, stroke protocol | Retinal infarction in <2 h |
| Angle-Closure Glaucoma | Pain, halos, nausea, firm eye | Acetazolamide 500 mg + same-hour referral | Optic nerve ischemia |
| Retinal Detachment | Flashes, floaters, curtain | Protect eye, same-day surgical referral | Prevents macular loss |
| Corneal Ulcer | Pain, opacity, photophobia | Stop lenses, no steroids, urgent referral | Prevents corneal melt |
| Endophthalmitis | Post-op pain, vision loss, hypopyon | Emergency referral, no delay | Intraocular sepsis |
Practical GP Pearls
- Always test visual acuity — even grossly reduced vision matters for triage.
- Check pupils for RAPD; document red reflex when visible.
- Don’t be misled by minimal redness — CRAO and detachment can look quiet.
- Avoid topical steroids unless prescribed by ophthalmology.
- If unsure: “When in doubt, phone and refer out.”
Key Takeaway
The eye is the only part of the central nervous system directly visible to clinicians — and the window of opportunity for vision rescue is often minutes to hours. For each of these five emergencies, rapid recognition and immediate referral are the difference between full recovery and irreversible blindness.
Early, confident escalation from general practice or casualty care can save sight and preserve quality of life.